In New York, cannabis advocates and businesses are weighing the recent expansion of the state’s tightly regulated medical marijuana program.
Last month, the Department of Health added opioid use, chronic pain and post-traumatic stress disorder (PTSD) to the list of qualifying conditions under the state’s medical marijuana program, which was among several recent improvements to the program, according to Jill Montag, department spokesperson.
On July 12, the department officials published emergency regulations for the opioid replacement policy, adding “any condition for which an opioid could be prescribed as a qualifying condition for medical marijuana,” according to the state’s website.
On top of the newly added qualifying conditions, the Department of Health also greenlit five more manufacturers and dispensaries in the state—and opened the door to home delivery regulation.
“The Department of Health is committed to growing New York’s Medical Marijuana Program responsibly,” Montag told Cannabis Business Times.
The Marijuana Policy Project (MPP) was one of the organizations supporting the addition of PTSD to the program, according to general counsel Kate Bell. “We were obviously excited that they added that as a qualifying condition, and the Health Department has done a number of other things over the past almost two years now to try to expand the program,” Bell said. “New York used to be one of the most restrictive programs in the country, and it is improving. There are still … more improvements that could be made, but it definitely has gotten better in recent times.”
As of July 3, there were 61,699 certified patients and 1,725 registered practitioners participating in the program, Montag said.
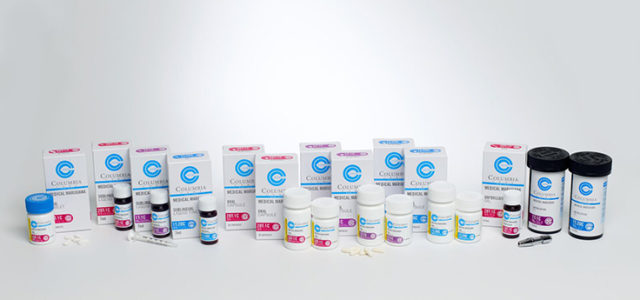
“New York was obviously one of the achievements we’re most proud of as an organization,” said Nicholas Vita, CEO of Columbia Care, a multi-state medical marijuana operator with a license in New York. “We were able to partner very effectively with our local communities and develop a plan that reflected the wishes of not only the governor and the legislature, but that matched well with the expectation of the Department of Health. New York for us has become a crown jewel for manufacturing standards and excellence of quality that I think many, many markets in the United States ultimately would hope to be able to match.”

Columbia Care’s product offerings in New York. Photo courtesy of Columbia Care LLC.
Medical Marijuana vs. Opioids
The addition of opioid use to New York’s medical marijuana program is a victory for Dr. Ramesh Sawhney, a board-certified physician who co-founded The Recovery Spot, a drug addiction treatment center New York City, with his partner, Dr. Scott Bienenfeld.
“As far as the opioid patients, they clearly want to use medical marijuana in lieu of opioids,” Sawhney said. “One is lethal and the other is non-lethal. The advantage of medical marijuana is going to save a lot of lives.”
And while New York may lack a scientific approach in the implementation of its medical marijuana program, according to Sawhney, The Recovery Spot looks at it a little differently. “This is really a clinical, medical, scientific approach to a problem that has never had a scientific approach until now,” Sawhney said. “The medical marijuana industry is controlled by non-scientists and non-physicians, and in order to realize the true impact of what’s occurring with medical marijuana, you need to incorporate a scientific approach, which means that you need to look at and address every patient, you need to quantify, you need to have the data.”
Sawhney and Bienenfeld saw a need for the use of medical marijuana in New York’s opioid-addicted population and sought to have the condition added to the state’s list of qualifying conditions. “This was put in front of the state Senate and the governor almost two years ago, at which time they denied it,” Sawhney said. “So now they’re revisiting it, partially because Pennsylvania has opened the doors, and I think the competing states are now saying, ‘Yeah, this is one of the treatment protocols and it should be allowed,’ so New York is starting to revisit that and it’s starting to gain more acceptance.”
Improving Patient Access
However, the addition of new qualifying conditions to the program and other improvements may not be enough to improve patient access, according to David Holland, principle of the Law Offices of David Clifford Holland and executive and legal director of Empire State NORML. “It’s still a pretty restrictive program, relative to other areas of the country,” he said. “It’s not readily accessible to a lot of people, and the more rural areas of New York state are not well serviced. They’re not closely situated to facilities, and therefore it’s not in the success story, in my opinion, in that we would’ve liked to have seen.”
Each of the ten licensees in the program has a cultivation facility and four retail outlets, and although the licenses have been doubled from five to ten, Holland said more are still needed. “That’s slightly more than one legal facility per million people,” he said. “New York has 30 million people, so we’re not having a high density … in this area.”
With the additional qualifying conditions, it may seem that the patient demand would outgrow the limited supply even further, but Vita said demand has remained consistent. “I think demand across all of the qualifying conditions has been pretty consistent and fairly robust,” he said. “The inclusion of any additional qualifying conditions I think has a compounding effect to that baseline growth level, but if you look at our demographics, if you look at the qualifying conditions, there’s a very, very balanced portfolio of patients and clinicians who have chosen to support, enroll or participate in the program statewide.”
The limited number of licensees in the state may also keep prices high for patients, Bell said. “Having robust competition ensures reasonable prices,” she said. “The government is creating an artificial oligopoly as it’s going to increase prices. So, that’s an issue.”
And more dispensaries may not completely solve the problem, Bell added. “Dispensaries alone don’t address the competition issue if they’re all owned by the same companies,” she said.
The high prices are also a reflection of the state’s ban on whole plant access, Bell said. “All of that processing adds cost,” she said. “They finally allow some limited whole plant, but it’s not for smoking—it’s ground up, and it’s still not the same as just allowing people to have flower, which makes it much cheaper for patients and then therefore gets more people into the program.”
Top Image: © Atomazul | Adobe Stock
MJ Shareholders
MJShareholders.com is the largest dedicated financial network and leading corporate communications firm serving the legal cannabis industry. Our network aims to connect public marijuana companies with these focused cannabis audiences across the US and Canada that are critical for growth: Short and long term cannabis investors Active funding sources Mainstream media Business leaders Cannabis consumers








